
Sleep Health, Sleep Disorders & Conditions
January 11, 2022
Sleep Apnea Guide: The Best Tips for Sleeping With Sleep Apnea
Written by Rebecca Renner
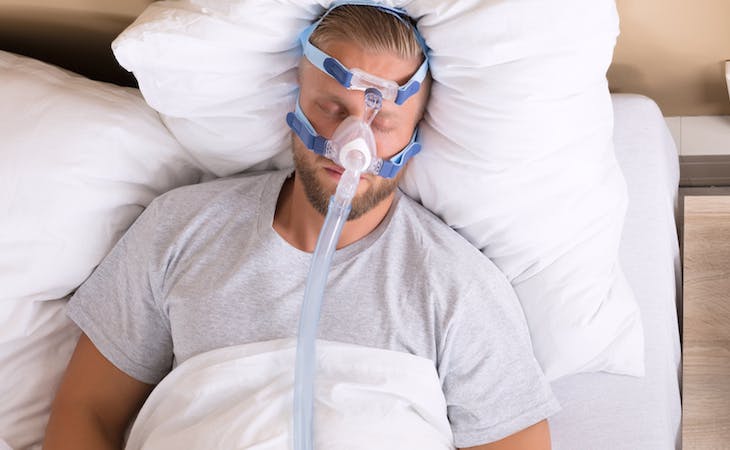
Sleep apnea is a common sleep disorder that causes breathing cessation during sleep. It can be life-threatening and is associated with an increased risk of serious conditions. Sleep apnea can affect anyone, including women. Common signs include snoring, lack of focus, pauses in breathing, morning headaches, and daytime sleepiness. Diagnosis can be done through a sleep study or a home sleep test. Treatment options include using a CPAP machine, maintaining good sleep hygiene, and considering other therapies.
Have you been waking up exhausted? If you think you’ve been getting a full night’s sleep but you still feel terrible in the morning, you could have sleep apnea, a common sleep disorder that causes you to stop breathing while you’re sleeping, possibly many times a night.
Those brief periods of breathing cessation are called “apneas.” During an apnea, the muscles in your tongue and the back of your throat relax, causing your airway to narrow or become blocked when you breathe in.
Sleep apnea is more than just a nuisance. It can be life-threatening, and it’s associated with an increased risk of other serious conditions such as heart disease, diabetes, high blood pressure, and stroke.
Because sleep apnea affects your ability to get adequate deep sleep, even driving when you have this condition can be deadly. So if you suspect you may have sleep apnea, tell your doctor right away.
Here, learn more about the common signs of sleep apnea, what getting a sleep apnea diagnosis looks like, and how to sleep better with sleep apnea.
What is sleep apnea?
Sleep apnea occurs when the muscles in a person’s throat relax, blocking the airway and causing a momentary cessation of breathing. The person then wakes up, gasps for air, and goes back to sleep.
The sleep apnea process can repeat hundreds of times a night, preventing the body from entering deep sleep and depriving it of much-needed oxygen.
This can result in high blood pressure, leading to an increased risk of heart attack and stroke.
Types of sleep apnea
There are three different types of sleep apnea: obstructive sleep apnea (OSA), central sleep apnea (CSA), and a combination of both.
OSA is the most common type of sleep apnea, and it happens when your tongue, tonsils, or other tissues in the back of your throat block your airway.
For people with OSA, sleep is restless and marked by shallow breathing and then pauses in breathing lasting 10 to 30 seconds. These pauses are often followed by jolts, coughs, snorts, and gasping sounds as the person tries to start breathing again, which can be quite alarming for anyone else in the room.
CSA is a little different. It occurs when the brain fails to send a signal to the muscles to breathe.
Sometimes, obstructive and central sleep apnea go on at the same time. This is called complex sleep apnea syndrome.
Who is at risk for sleep apnea?
Obstructive sleep apnea is on the rise in the United States. That’s mostly because the population is getting older and more obese, two major risk factors for the condition.
The people most likely to suffer from sleep apnea are older, overweight males—particularly African Americans, Pacific Islanders, or Hispanic men.
However, the full range of risk factors is broad and complex. Other risks include sedative or alcohol consumption, having a small or recessed jaw, a narrow airway, large tonsils, a large uvula, or a wide neck.
Bottom line: anyone—even high-performing athletes—can suffer from sleep apnea.
Can women have sleep apnea too?
“A common misconception is that sleep apnea only inflicts overweight, mature males,” says Kent Smith, DDS, board-certified dental sleep medicine specialist and president of the American Sleep and Breathing Academy. “While it is true sleep apnea is often diagnosed in males, and that obesity and age are both risk factors, sleep apnea is becoming increasingly diagnosed in people of all ages, including children.”
Female patients may have more trouble realizing they have sleep apnea because many women snore less loudly than men do. In other words, your partner might not notice when you’re having apneas while you sleep.
Smith advises female patients to watch out for additional symptoms, including depression, anxiety, and Restless Legs Syndrome (RLS). If you experience these symptoms, in combination with daytime sleepiness or inability to stay asleep, make an appointment to see your doctor.
How do I know if I have sleep apnea?
According to Smith, “the list of signs associated with sleep apnea is long and can vary widely for each person.”
However, Smith does advise patients and their loved ones to watch for these most common signs:
- Loud or persistent snoring
- Lack of focus/inability to concentrate due to fatigue
- Silent pauses in breathing while asleep
- Nighttime gasping, coughing, or choking
- Morning headaches
- Difficulty staying asleep
- Irritability, depression, or mood swings
- Dry mouth or sore throat upon awakening
- Frequent need to urinate during the night
- Dozing off while driving or doing other daily activities
- Insomnia of unknown origin
- Night sweats
Loud, chronic snoring is definitely the strongest sign of sleep apnea. The tissues at the back of the throat vibrate as they struggle to let air through, and the result is snoring (followed by those snorting and gasping sounds). But it’s important to note not all snorers have sleep apnea. (Learn why drooling could be a symptom of sleep apnea.)
How to diagnose sleep apnea
Suffering in silence seldom gets anything done. The first step toward getting a better night’s rest is to talk to your doctor, who can refer you to a sleep specialist.
A sleep specialist will schedule a sleep study. During a sleep study, you may be asked to sleep in a clinic where technicians and nurses can monitor your breathing.
Before you go to bed, they will hook you up to sensors that will show if you stop breathing during the night and for how long. Other sensors will measure sleep quality factors, including how long you maintain REM (rapid eye movement) sleep. The doctor will be able to diagnose your condition based on these readings.
It’s also possible to do a home sleep test that can give your doctor much of the same information with less inconvenience and cost to you (a home sleep test usually costs around $300, and many insurance programs including Medicare cover them).
How a home sleep test for sleep apnea works
After picking up the home sleep test equipment from your doctor, you simply apply the sensors, attach the clip to your finger, put an airflow sensor under your nose, turn on the monitor, and go to sleep as you usually do.
The home sleep test records your oxygen saturation, heart rate, airflow, movement in your chest and abdomen, sleep positions, and even the time you spend snoring.
The next day you simply return the device to your doctor. The data collected by the device is immediately available for interpretation. That means you will be able to know quickly what your course of action needs to be.
The limits of home sleep tests
A home sleep test won’t necessarily provide the extensive results you get from a traditional sleep study in a lab.
In addition to everything the home test records, a sleep lab study also measures brain waves, sleep time, and leg movements that would indicate RLS. You also won’t have staff to make sure you properly connect everything. And it may not be right for you if you have coexisting health issues such as congestive heart failure or pulmonary disease.
That said, “Many of the portable devices currently available show a lot of promise with producing information that is in line with what we see in the lab,” says Charlene Gamaldo, MD, medical director of Johns Hopkins Center for Sleep at Howard County General Hospital in Maryland.
In fact, Johns Hopkins already uses several FDA-approved at-home devices for measuring sleep brain wave activity, assessing leg movements, and monitoring breathing.
How can I sleep better with sleep apnea?
If you’ve been diagnosed with sleep apnea, here are some strategies for scoring better shuteye.
Choose the best sleep position for sleep apnea
Sleeping on your back is the worst position for breathing disorders like sleep apnea and snoring. That’s because lying supine can allow your soft palate to relax and block your airway.
Side-sleeping, on the other hand, is less likely to result in obstruction. You’ll probably need a softer mattress for this to work because side sleeping puts the greatest amount of pressure on your hips and shoulders.
Stomach sleeping can work too, but that’s the worst position for your back. If you have trouble staying off your back, some doctors suggest sewing a tennis ball into the back of your pajama shirt. Drastic, we know, but it works!
An elevated head is another sleep position that can help mitigate sleep apnea while you snooze. You can raise your head with pillows or an adjustable bed base.
Invest in a CPAP machine
If your sleep doctor determines that you have sleep apnea, they’ll most likely prescribe an apparatus called a CPAP machine, which stands for continuous positive airway pressure. CPAP machines work by sending a constant flow of air into your throat, causing your airway to stay open while you sleep.
Clean your CPAP regularly
Your CPAP sits by your bedside all day, gathering dirt, dust, and grime. If you have a humidifier, that moisture makes a CPAP even more inviting for bacteria.
At least once a week, in the morning, dunk your CPAP paraphernalia in soapy water, and—this is crucial—give it the best part of a day to dry. Hang the tubing so the water can drip easily from both ends as it dries.
You can wash your mask cushion more frequently. At the very least, keep some baby wipes handy and give the cushion a swipe every night before bed. A dirty cushion won’t seal properly, shifting and making noise throughout the night.
Maintain your CPAP like any other piece of machinery
The CPAP is partly mechanical, so it can be finicky. Pay attention to how it sounds every night, and note anything unusual.
Make sure to check and replace the filters, as this can contribute to noise and faults with the motor. If you travel with your CPAP, check it after every flight. Jostling and shaking can damage the motor. See if your insurance will cover a replacement in case of mechanical failure.
Plan for the unexpected
Relying on a CPAP reminds you of how much you take other necessities for granted: electricity and bottled water, for instance. Consider buying a portable power supply and extension cord in case you lose power during a storm.
Also, in some places, distilled water can be hard to come by. It’s a good idea to carry a decent supply of the stuff before you set out on a road trip. Pro tip: deionized water, available from most mechanics, works in a pinch.
Resist the urge to use tap water, especially in places with “hard” water supplies, unless you want to be scrubbing grime from your humidifier chamber for the first 30 minutes of your day.
Be realistic with your CPAP expectations
A CPAP isn’t a magic cure for all sleep problems. You still need to maintain an otherwise healthy lifestyle, especially if you have some of the underlying conditions that lead to sleep apnea in the first place.
Don’t get complacent. Once the initial euphoria of a full night’s worth of oxygen wears off, you’ll encounter the same issues that everyone faces: good nights, bad nights, decisions you’ll regret in the morning.
CPAP therapy will get you to a place where you can have a normal, functioning life—but the rest is on you.
Do exercises to strengthen your airway
Believe it or not, singing regularly may help with sleep apnea. So make sure you crank up the radio and bust out some tunes whenever you can.
Consider other therapies
CPAPs are considered the “gold-standard treatment” by experts like Smith. Your doctor will probably ask you to try the CPAP machine before exploring other options.
But if that doesn’t improve your sleep apnea, other therapies include oral appliance therapy and surgery. Work with your doctor to determine what works best for you. (Here’s why you shouldn’t try mouth taping for sleep if you have sleep apnea.)
Sleep apnea FAQs
What is obstructive sleep apnea?
OSA is the most common type of sleep apnea. It occurs when your tongue, tonsils, or other tissues in the back of your throat block your airway. People with OSA often experience restless sleep marked by shallow breathing and then pauses in breathing that last 10 to 30 seconds. These pauses are usually followed by jolts, coughs, snorts, and gasping sounds as you try to start breathing again.
Is sleep apnea genetic?
Genetics play a role, but the causes of sleep apnea are complex. This condition is typically the result of a combination of genetics, health, and lifestyle factors.
Is sleep apnea dangerous?
Sleep apnea is a serious medical condition that can be quite dangerous if left untreated. It’s linked with an increased risk of other serious medical conditions, like heart disease, diabetes, high blood pressure, and stroke. Plus, studies show people with untreated sleep apnea are at higher risk of fatigue-related car crashes since they don’t get enough deep sleep during the night. If you think you might have sleep apnea, consult your doctor ASAP because it can be life-threatening.
Can sleep apnea be cured?
There is no cure for sleep apnea. However, CPAP machines and oral appliances work well to keep this condition under control. Additionally, if your sleep apnea is caused by excess weight, then losing weight may help alleviate symptoms.
Can you use a weighted blanket with sleep apnea?
It’s best to avoid the use of weighted blankets if you have sleep apnea. That’s because a weighted blanket can further restrict breathing. Anyone with a chronic respiratory or circulatory condition should avoid using a weighted blanket.
What aggravates sleep apnea?
Sleeping in certain positions (such as on your back), too much alcohol consumption, weight gain, and getting older (we know, it’s something you can’t avoid!) can all aggravate sleep apnea and make symptoms worse.
How can I sleep with sleep apnea without a CPAP?
The main treatment for sleep apnea is the use of a CPAP machine. However, these devices can be clunky and uncomfortable, and in some cases, they don’t work for OSA symptoms.
There are a few alternative options to CPAP therapy. These include oral appliances, bilevel positive airway pressure (BiPAP), nasal valve therapy, lifestyle changes like losing weight and quitting smoking, and surgery to fix underlying causes of sleep apnea. Always consult with your doctor before starting a new sleep apnea treatment.
Find the best mattress for sleep apnea at Saatva
Getting sleep apnea under control isn’t always easy. While using a CPAP machine is the most common and effective treatment for sleep apnea, your sleep position and mattress can also help mitigate some of the symptoms.
If you have sleep apnea, it’s best to sleep on your side or with your head elevated in bed to help keep your airway open while you sleep. Saatva offers a variety of high-quality mattresses that are suitable for side sleepers, as well as an aadjustable bed base that makes it easy to raise your head and find the perfect position.
Take our online mattress quiz to find out which one of our mattresses is right for you. All of our mattresses come with a 365-night home trial so you test one out before deciding.
Rebecca Renner
Rebecca Renner is a journalist who’s been published in The Washington Post, The Atlantic, Outside Magazine, and National Geographic.






